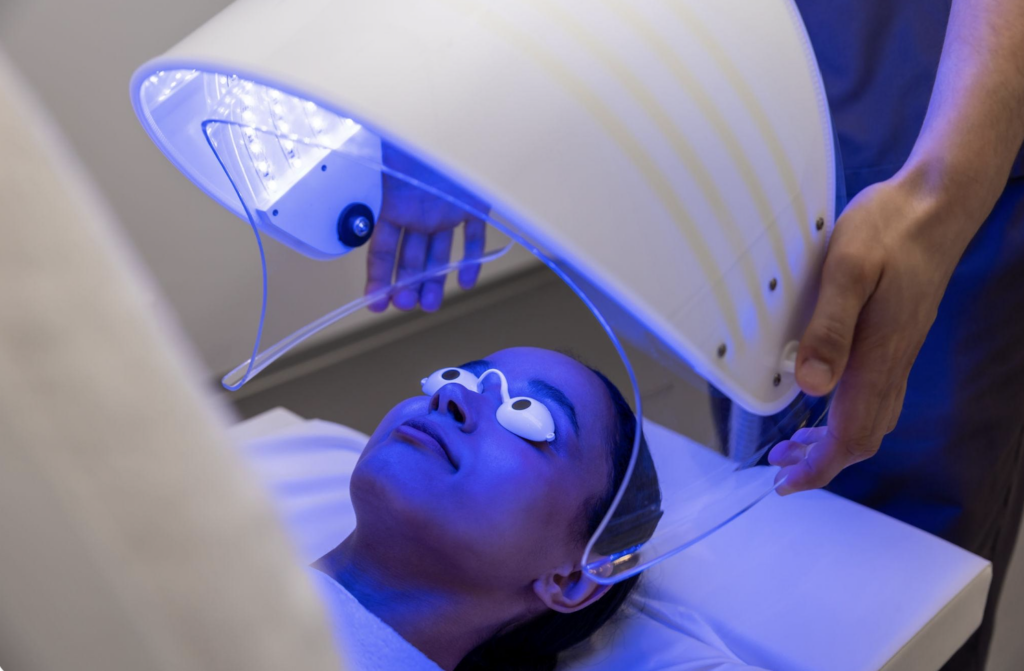
For patients researching laser-based approaches frequently used in the care of melasma, the priority is usually clarity. Melasma is a common skin condition marked by grayish-brown patches or other uneven areas of discoloration, most often on the face, and it tends to appear in sun-exposed areas such as the cheeks, forehead, and upper lip. It is especially common in women, often connected to sun exposure, hormonal changes, and other long-term triggers that make pigment return even after improvement.
That pattern is one reason many people eventually look beyond topical treatments and start reading about laser treatments, laser therapy, and other office-based options. Even so, experienced dermatology sources emphasize that there is no single best way to treat melasma for every patient. Treatment plans are usually built around sun protection, topical medication, trigger management, and carefully selected procedures rather than one stand-alone fix.
This distinction matters in a medical spa setting. Patients often arrive wanting an effective treatment for brown spots, stubborn pigmentation, or visible discoloration that has not responded to over-the-counter products. A thoughtful consultation should frame melasma as a chronic pigment disorder that may improve with treatment but can also flare again, especially with ultraviolet light, visible light, heat, or ongoing hormonal influence.
Sun Protection and Trigger Control Remain Central to Melasma Treatment
Before discussing devices, it is important to state what most authoritative guidance already makes clear: sun protection is foundational in melasma treatment. The American Academy of Dermatology notes that sunlight causes the skin to make more pigment, which can darken existing melasma and lead to new patches, and it recommends broad-spectrum sunscreen along with shade and protective habits.
In practical terms, patients who pursue procedures without consistent protection may find that their melasma becomes active again quickly. That is why clinicians often advise patients to avoid direct sun exposure, practice strict sun protection, and continue protective routines even when the skin looks clearer. In many cases, the visible progress from a procedure depends just as much on what happens between visits as what happens in the treatment room.
Trigger review also matters because melasma may worsen with birth control, pregnancy-related shifts, and other hormonal triggers. DermNet notes that melasma has been linked to estrogen- and progesterone-containing contraceptives, implants, and hormone therapy, while the AAD also identifies medications and sunlight as relevant contributors. When melasma is influenced by ongoing triggers, any treatment for melasma should be framed as management rather than permanent removal.
Topical and Combination Care Usually Come Before Energy-Based Procedures
Most patients do not start with lasers, and that is often appropriate. The AAD explains that treatment frequently combines sun protection with medications applied to the skin, and many patients begin with prescription or physician-guided products before moving to procedural care. That makes room for topical creams, other topical treatments, and selected skin lightening agents to address excess pigment more conservatively before a device is introduced.
This stepwise approach is especially important in patients with darker skin tones, recent inflammation, or a history of pigment rebound. If the skin barrier is irritated or if the diagnosis is not fully clear, aggressive treatment can increase the risk of post-inflammatory hyperpigmentation rather than improve the original problem. For that reason, pre-treatment planning usually matters as much as the procedure itself.
At BluePoint Medical Spa, this broader context is relevant because the spa offers cosmetic procedures such as chemical peels, laser treatments, and IPL-based photo facials for pigmentation-focused concerns. Those services can be part of a longer strategy, but they should be matched to diagnosis, skin type, pigment depth, and recovery tolerance rather than chosen simply because a laser sounds stronger.
Intense Pulsed Light Is a Light-Based Option With Careful Patient Selection
Although not a true laser, intense pulsed light is often included in discussions of light therapy and energy-based pigmentation care. DermNet notes that IPL is used for pigmented lesions and discolouration problems such as melasma, and BluePoint’s current menu includes Photo-Facial (IPL) as one of its available treatment options.
For some patients, IPL appeals because it is commonly associated with minimal downtime, broad treatment coverage, and visible brightening in superficial pigment concerns. It may also be considered when there are mixed goals involving redness, tone irregularity, or textural refresh. In the right context, this kind of skin rejuvenation can improve the overall look of the complexion, especially when melasma overlaps with photodamage.
Still, IPL is not a simple answer for every case. DermNet also cautions that physical treatments such as laser treatments and IPL may aggravate pigmentation by injuring the epidermis, and this matters even more in reactive skin or in patients with a tendency toward rebound darkening. For melasma-prone skin, careful diagnosis, conservative settings, and expectation management are essential.
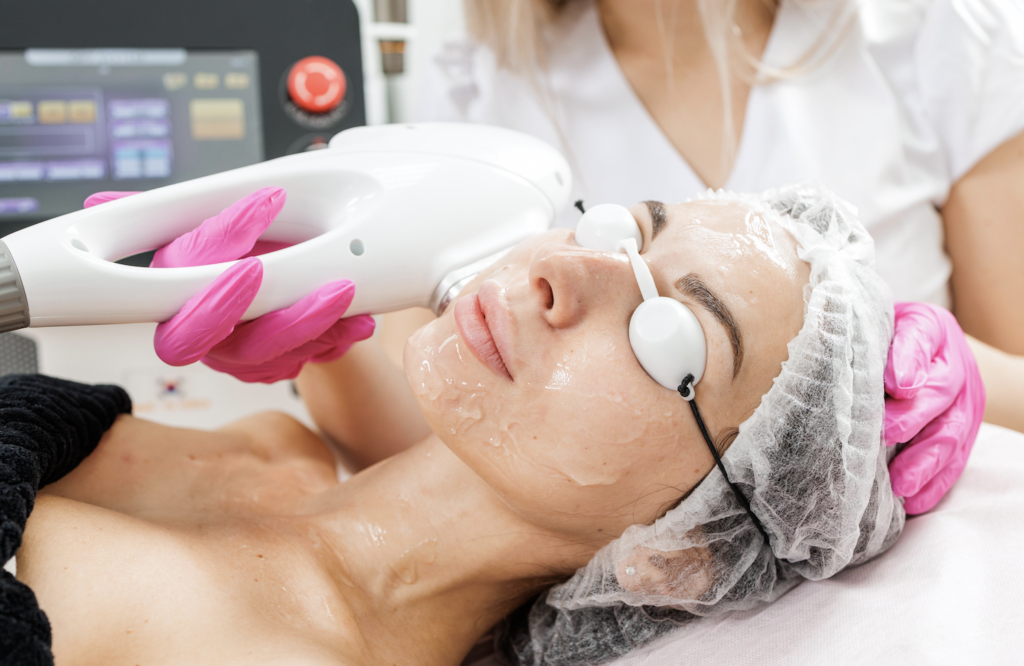
Q-Switched Nd: YAG Lasers Are Often Discussed for Resistant Melasma
Among the better-known laser types used in melasma care, q switched nd: YAG devices—especially low-fluence 1064 nm approaches—appear frequently in the literature for resistant melasma and stubborn or dermal melasma. Review literature summarized in PubMed Central notes that low-fluence Q-switched Nd: YAG may be one of the more useful options for refractory melasma, particularly in patients with darker skin types when settings are chosen carefully.
This is one reason terms such as Q-switch laser, YAG lasers, and different lasers appear so often in melasma education. A longer wavelength may reduce some epidermal risk compared with more aggressive resurfacing approaches, which is relevant when the patient has more melanin in the epidermis. In real practice, however, the device alone does not determine safety; patient history, trigger control, technician expertise, and pre- and post-care all affect the outcome.
Patients should also know that a Q-switched protocol is usually not a single treatment solution. Multiple treatment sessions are more typical, and improvement can still be partial or temporary if triggers remain active. That is why this category is usually presented as part of a broader plan to address melasma, not as a stand-alone cure.
Fractional and Non-Ablative Lasers Are Used With a Different Goal
Fractional lasers are often discussed when the goal includes both pigment and remodeling. Some devices aim to create controlled microscopic injury while leaving untreated tissue around the columns, which may support healing in the surrounding skin and may also stimulate collagen production. That dual effect explains why these devices are sometimes considered when melasma coexists with textural concerns or a desire for broader skin rejuvenation.
Within this category, non-ablative lasers generally attract interest because they tend to involve less surface disruption than ablative lasers. That lower level of injury can be important when patients want minimal downtime or when the provider is trying to reduce the likelihood of pigment worsening after treatment. Even so, lower downtime does not mean zero risk, especially in melasma-prone skin.
By contrast, more aggressive resurfacing can produce more thermal damage, and review literature has warned that ablative fractional lasers should be used cautiously because of higher risks of hypo- and hyperpigmentation. For patients with darker skin, that caution becomes even more important, because inflammation itself may leave the skin darker during the recovery process before it looks better.
Darker Skin Tones Require Extra Caution and More Conservative Settings
Melasma care in darker skin tones deserves particular attention because melanin competes for energy absorption during many laser and light procedures. DermNet explains that skin of color develops pigmentary changes more readily after injury or inflammation, and that melanin can increase the risk of side effects after epidermal injury by a laser.
That concern becomes especially relevant in Fitzpatrick skin types, including patients described in many practices as Fitzpatrick skin types IV and above, depending on the device and treatment target. Conservative settings, cooling, test spots, and shorter sessions may reduce risk, and recent Dermatology Times commentary on melasma protocols in darker skin stresses careful patient selection, cooling, and conservative parameters to minimize post-inflammatory hyperpigmentation.
This is also why not every device is equally favored for every patient. Some wavelengths and techniques are approached more cautiously in darker skin, especially if the patient has active tanning, recent inflammation, or a history of rebound pigment after peels or lasers. Personalization is not just a preference in melasma care—it is a safety strategy.
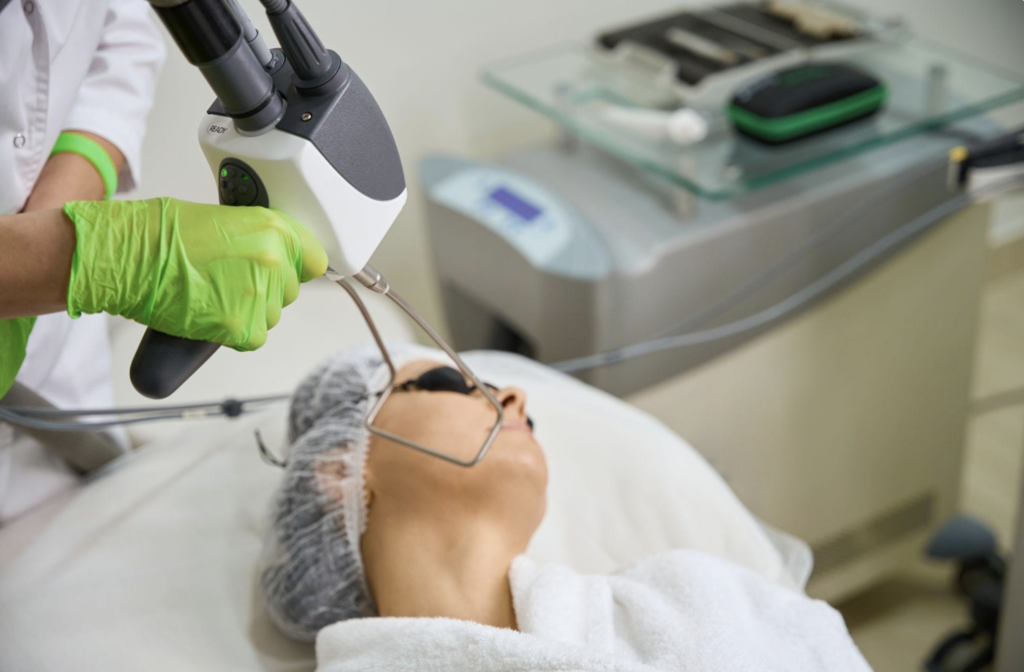
Picosecond Lasers and Other Emerging Options Are Part of the Ongoing Conversation
Newer conversations about melasma often include picosecond lasers, particularly because clinicians are interested in whether very short pulse durations may fragment pigment with less collateral heat. Recent reviews and summaries note that picosecond technologies are part of the expanding melasma literature, although outcomes still depend on patient selection, protocol design, and ongoing maintenance.
That does not mean newer is always better. In melasma, recurrence remains a major issue regardless of device age, and some patients respond better to thoughtful combination care than to a newer machine used in isolation. For patients with mixed-type melasma, dermal melasma, or pigment that appears deeper in the deeper layers of the skin, realistic counseling matters more than marketing language.
Because melasma is influenced by visible light, heat, inflammation, and hormones, some providers combine device-based care with brightening agents, antioxidant support such as vitamin C, calming products, and home-care planning. Patients may also ask about soothing ingredients such as aloe vera, but supportive skincare should be presented as adjunctive rather than as a replacement for medical diagnosis and pigment management.
Combination Plans Often Matter More Than a Single Device Choice
One of the clearest themes in modern melasma care is that other treatments are often used alongside energy-based procedures. That may include continued topical therapy, carefully timed chemical peels, and pigment-control products before and after treatment. For some patients, the best results come from sequencing therapies rather than pushing one device harder.
This matters because laser outcomes in melasma are often gradual. Some patients need a series rather than one visit, and common clinical language around pigment devices often involves three to four sessions or other repeated treatment schedules, depending on the technology, response pattern, and downtime tolerance. In melasma, repeated but conservative care may be safer than a single aggressive intervention.
When vascular redness seems to overlap with pigmentation, clinicians may also consider whether vascular components are contributing to the appearance of the discoloration. Even then, device choice should still be grounded in diagnosis, because treatments that seem appealing for redness or tone correction may not be the most suitable for melasma-prone skin.
Post-Treatment Care Strongly Influences How the Skin Looks Afterward
Patients often focus on the procedure itself, but post-treatment behavior frequently shapes the final cosmetic result. After IPL, DermNet advises patients to avoid sun exposure before and after treatment, and similar logic applies more broadly across many pigment procedures. When the skin is inflamed, even brief direct sun exposure may contribute to recurrence or darker healing in the treated areas.
Aftercare usually includes gentle cleansing, barrier-supportive products, and temporary avoidance of irritating actives, depending on what was done. That is also the stage when patients need to understand that melasma may look uneven before it looks better, especially if transient inflammation develops in the skin after treatment. A calm explanation of expected changes can reduce unnecessary anxiety and improve adherence.
Providers should also review whether a patient is taking certain medications, using potentially irritating brighteners, or dealing with ongoing endocrine or reproductive factors that may keep reactivating pigment. The procedure may be brief, but melasma management is rarely brief. Long-term improvement usually depends on what happens after the visit as much as what happens during it.
The Appropriate Treatment Depends on Diagnosis, Skin Type, and Expectations
When patients ask which device is best, the most accurate answer is usually that the appropriate treatment depends on the diagnosis, pigment depth, prior response history, skin tones, trigger pattern, and willingness to continue maintenance care. Superficial pigment, mixed-type melasma, and deeper or more stubborn pigmentation do not all behave the same way, and treatment should reflect that difference.
This is where the value of a qualified dermatologist or licensed provider-supervised evaluation becomes clear. The AAD recommends dermatologist involvement because melasma can resemble other pigment disorders, and diagnostic tools such as a Wood’s lamp or dermatoscope may help show how deeply pigment reaches. That information can change whether a patient is steered toward procedures, prescription products, or a slower maintenance-first plan.
BluePoint Medical Spa offers laser and light-based services within a broader aesthetic menu, including IPL and exfoliation-based services, which makes consultation especially important for patients in Las Vegas who are comparing options for pigmentation care. Elective aesthetic treatment should be chosen with realistic expectations, careful review of risks, and clear discussion of whether the concern appears more superficial, more inflammatory, or more consistent with classic melasma.

FAQ
Are Laser Treatments Always the First Step for Melasma?
No. Many treatment plans begin with sun protection and physician-guided topical care, with procedures added later when appropriate. Lasers and light devices are usually considered part of combination care rather than the universal first choice.
Can Darker Skin Tones Be Treated Safely With Laser Therapy?
Sometimes, but the margin for error is smaller. Conservative settings, cooling, and careful device selection matter because darker skin types have a higher risk of pigment change after inflammation or thermal injury.
Does IPL Work the Same Way as a Laser for Melasma?
No. IPL is a broad-spectrum light treatment rather than a single-wavelength laser, even though it is often discussed alongside laser-based options. It may be used for pigmented concerns, but suitability depends on diagnosis, skin tone, and sensitivity.
Will One Session Remove Melasma Completely?
Usually not. Melasma often needs repeated care, ongoing trigger control, and strict sun protection, and recurrence is common. A single session may improve appearance, but long-term management is usually more realistic than permanent removal.
Conclusion
The top message for patients is that laser and light procedures may play a role in melasma care, but they work best as part of a larger plan that includes diagnosis, trigger review, maintenance, and rigorous photoprotection. Maintenance treatments are often necessary, and even great improvement does not guarantee that melasma will stay away if hormones, heat, or ultraviolet exposure continue to stimulate pigment production.
These services are elective, not medically necessary, and they should be approached with caution in patients prone to rebound pigment. Individual results vary, treatments carry potential risks or contraindications, and a consultation with a licensed provider is required before deciding whether a laser- or light-based procedure is appropriate. To discuss melasma treatment options, including IPL and related pigmentation-focused services, schedule a consultation with BluePoint Medical Spa.